CNN
—
The Trump administration announced Friday that it is not moving forward with a Biden-era proposal that would have expanded coverage of costly anti-obesity drugs to more than 7 million Americans on Medicare or Medicaid.
The Centers for Medicare and Medicaid Services did not explain why it was not finalizing the proposal, which the Biden administration unveiled in November.
However, the agency said in a statement that it may consider future policy options for anti-obesity medications “pending further review of both the potential benefits of these drugs including updated clinical indications, and relevant costs including fiscal impacts on stakeholders such as state Medicaid agencies.”
New US Health and Human Services Secretary Robert F. Kennedy Jr. has made statements strongly disapproving of the medications in the past, although his new CMS administrator, Dr. Mehmet Oz, frequently touted anti-obesity drugs on his television show and on social media. But expanding coverage would have been expensive, and the Trump administration and Elon Musk’s Department of Government Efficiency have said that slashing federal spending is one of their primary focuses.
Under the proposed rule, 3.4 million Medicare beneficiaries and about 4 million Medicaid recipients would have gained access to these medications, the Biden administration said in a fact sheet at the time.
Although Medicare by law is not allowed to cover drugs for weight loss, the Biden administration proposed reinterpreting the statute to allow coverage for the treatment of obesity as a chronic disease. Some 22% of Medicare enrollees were diagnosed with obesity in 2022, more than double the rate a decade prior.
The reinterpretation would also have applied to Medicaid, which means the mediations could not have been excluded from coverage when used to reduce excess body weight and maintain long-term weight reduction as a treatment for obesity.
Currently, 13 states cover GLP-1 medications for obesity treatment, according to KFF, a nonprofit health policy research organization.
However, the federal expansion would have cost Medicare an estimated $25 billion over a decade, the Biden administration said.
Broadening Medicaid coverage would have cost the federal government $11 billion and states $3.8 billion over a decade. State Medicaid agencies voiced “significant concerns over the fiscal impacts of this proposal,” the National Association of Medicaid Directors said in a letter to CMS in late January.
Even though the Trump administration has dropped the proposal, a growing number of Medicare and Medicaid beneficiaries are gaining coverage of the drugs, said Rachel Sachs, law professor at Washington University. That’s because the medications are also gaining approval to treat other conditions, such as heart disease and sleep apnea.
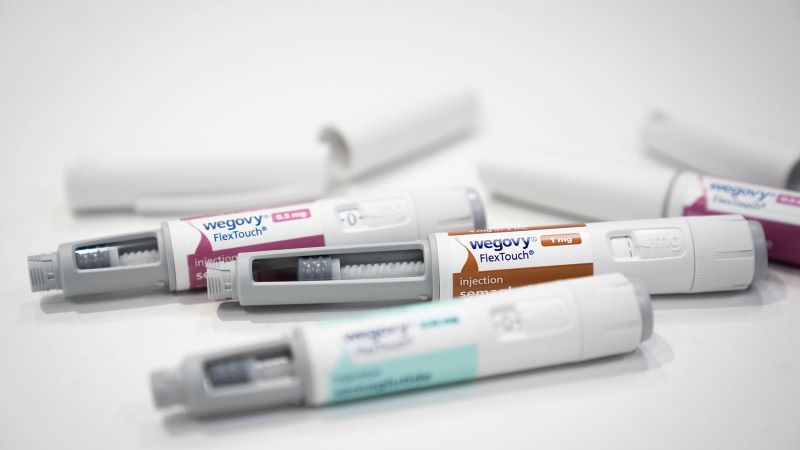
But the drugs are still out of reach for many beneficiaries. The list price for Wegovy, for instance, is nearly $1,350 for a four-week supply, although the manufacturer, Novo Nordisk, offers various discounts. Zepbound’s list price is more than $1,000, but Eli Lilly last year made starter doses available for between $399 and $529 for a four-week supply.
“We’re just back to the status quo, which is people on Medicare who need these drugs or want these drugs need to pay for them out of pocket,” said Juliette Cubanski, deputy director of KFF’s Program on Medicare Policy. “And given the high cost, that may be, for many people with Medicare, prohibitive in terms of access.”